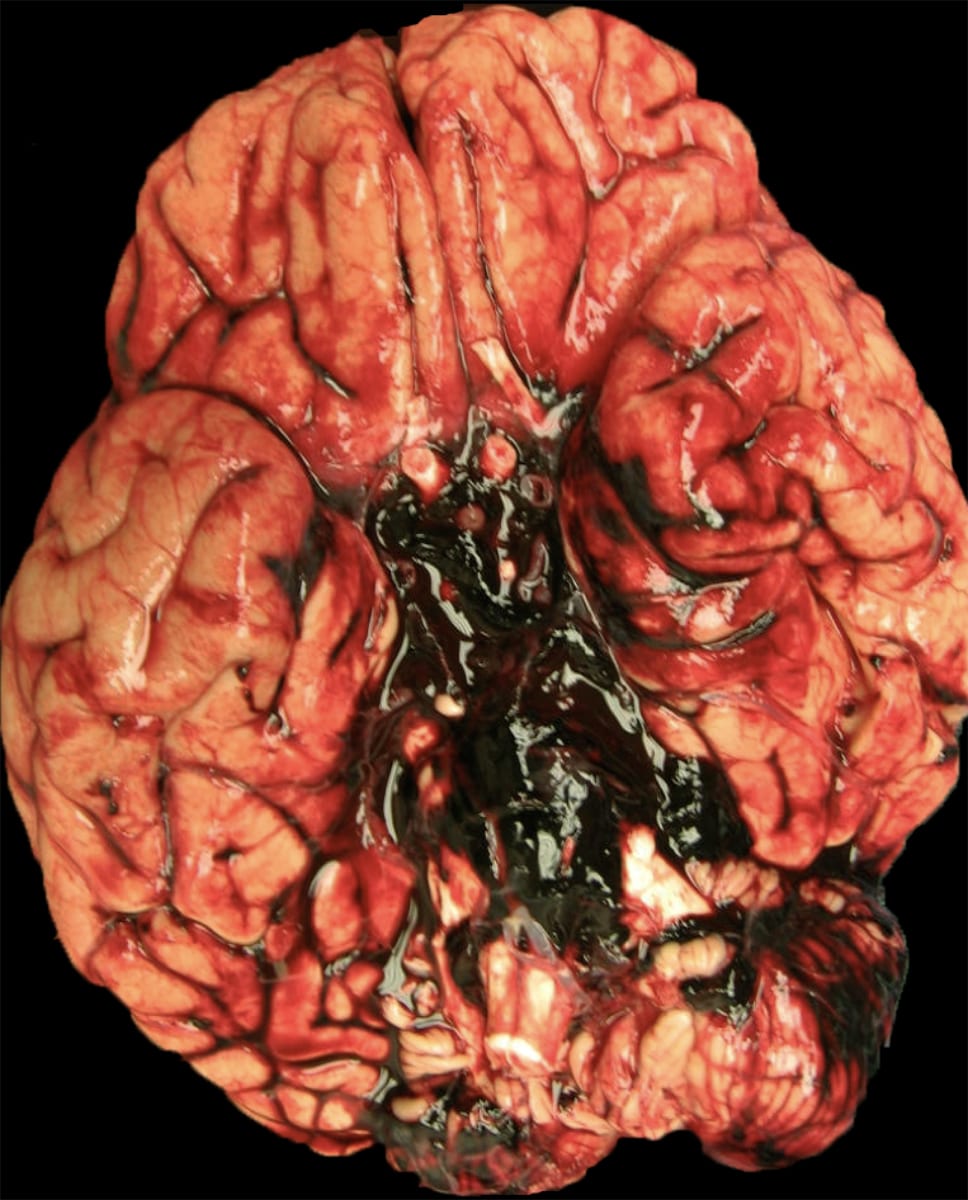
Picture this: it’s the 1980s, big hair is in, synth-pop is blasting, and neurologists are scratching their heads over how to best care for patients with subarachnoid hemorrhage (SAH). For most of the 1900s, treatment strategies that addressed the secondary complications of SAH included bed rest, blood pressure control, pain management, and early surgical intervention to secure an aneurysm if present. However, there was a significant gap in addressing delayed cerebral ischemia (DCI), a major cause of morbidity and mortality in SAH survivors.
Calcium channel blockers were researched for SAH patients due to their potential to prevent and treat cerebral vasospasm, which was thought to be the primary cause of DCI. Nimodipine, a dihydropyridine calcium channel blocker, was of particular interest due to its ability to cross the blood-brain barrier and its selective action on cerebral vessels. This theory led to the development of the “British Aneurysm Nimodipine Trial”. The goal of this study was to definitively assess whether this promising agent could improve outcomes in SAH patients, addressing a critical need in neurocritical care and potentially changing the standard of care for this devastating condition.
Published in 1989, The British Aneurysm Nimodipine Trial was a double-blind, placebo-controlled, randomized study that enrolled 554 patients across four regional neurosurgical units in the United Kingdom. These patients presented with acute SAH and were treated within 96 hours of symptom onset. The study compared the efficacy of oral nimodipine at a dose of 60mg every four hours for 21 days vs. placebo.
The results of the trial were compelling, with a lower rate of death or severe disability, at 6 months in the nimodipine group compared to the placebo group (17% vs. 33%, p = 0.0006). Those treated with nimodipine also had a lower incidence of cerebral infarction than the placebo group (22% vs. 33%, p=0.014). Additionally, adverse reactions to nimodipine, such as hypotension and elevated liver enzymes, were minimal and affected only a small proportion of patients. In summary, this data indicated that nimodipine use after SAH is not only associated with better outcomes than placebo but is also well-tolerated, further supporting its use in clinical practice.
In the following 35 years beyond this initial publication, multiple studies have continued to demonstrate the value of oral nimodipine over other therapies. For example, the 2020 NEWTON2 trial examined the value of intrathecal sustained-release nimodipine (EG-1962) for SAH but it was stopped early due to futility since it was unable to demonstrate superiority to angiographic vasospasm or better outcomes compared to standard oral nimodipine. The continued value of nimodipine in patients with SAH can be underscored by its consistent recommendation across multiple clinical guidelines, with major organizations including the American Heart Association/American Stroke Association and the Neurocritical Care Society strongly recommending oral nimodipine for all patients with aneurysmal SAH; nimodipine remains the only therapeutic agent with Class I evidence for decreasing the risk of poor outcome in aneurysmal SAH. Interestingly, it is important to note that nimodipine’s primary clinical benefit is not through reducing cerebral vasospasm as previously thought decades ago. Rather, it improves neurological outcomes by reducing DCI through mechanisms that are not fully understood.
In conclusion, nimodipine has proven it’s got more staying power than your favorite ’80s hairspray. Its unique position as the sole proven intervention for improving outcomes in SAH, coupled with its consistent endorsement across clinical guidelines, solidifies its status as an indispensable component in the management of this critical neurological condition. So, the next time you order nimodipine, remember: you’re not just prescribing a medication, you’re continuing a legacy that’s been rocking the neurocritical care world for over three decades!
- Pickard J D, Murray G D, Illingworth R, Shaw M D, Teasdale G M, Foy P M et al. Effect of oral nimodipine on cerebral infarction and outcome after subarachnoid haemorrhage: British aneurysm nimodipine trial. British Medical Journal 1989; 298 :636 doi:10.1136/bmj.298.6674.636
- Chou SH. Subarachnoid Hemorrhage. Continuum (Minneap Minn). 2021 Oct 1;27(5):1201-1245. doi: 10.1212/CON.0000000000001052. PMID: 34618758.
- Chung DY, Abdalkader M, Nguyen TN. Aneurysmal Subarachnoid Hemorrhage. Neurol Clin. 2021 May;39(2):419-442. doi: 10.1016/j.ncl.2021.02.006. Epub 2021 Mar 31. PMID: 33896527; PMCID: PMC8147706.
- Macdonald RL, Hänggi D, Ko NU, Darsaut TE, Carlson AP, Wong GK, Etminan N, Mayer SA, Aldrich EF, Diringer MN, Ng D, Strange P, Bleck T, Grubb R, Suarez JI. NEWTON-2 Cisternal (Nimodipine Microparticles to Enhance Recovery While Reducing Toxicity After Subarachnoid Hemorrhage): A Phase 2, Multicenter, Randomized, Open-Label Safety Study of Intracisternal EG-1962 in Aneurysmal Subarachnoid Hemorrhage. Neurosurgery. 2020 Dec 15;88(1):E13-E26. doi: 10.1093/neuros/nyaa430. PMID: 32985652.