Neuro-ophthalmology is a big field in neurology. In fact, it even has its own subspecialty! The pathways involved in vision and eye movements are just as fascinating as they are complex, and for this reason, test makers love to include questions on these topics! Test questions in these fields most often focus on neuro-anatomy and the physical exam and will be covered herein.
Authors: James Eaton, MD, Steven Gangloff, MD, and Brian Hanrahan, MD
Chapter Multimedia Content
Check out this chapter’s bonus multimedia content! Note, some of this content is only available to our full-access users.
Table of Contents
Table of Contents
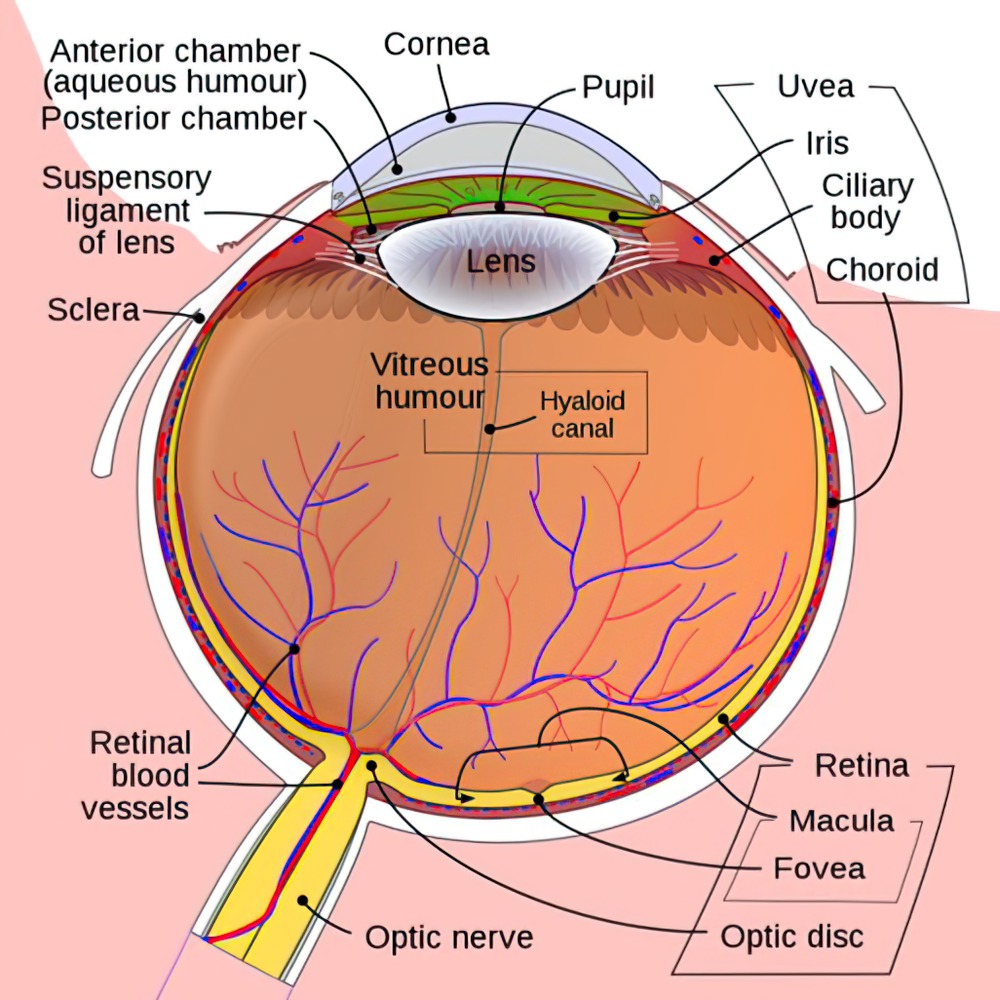
The Eye and Retina
- Light passes through the tear film, cornea, anterior chamber, lens, and posterior chamber before reaching the retina.
- Ciliary muscles change the shape of the lens to focus on objects at different distances.
- Once light reaches the retina, it then passes through the nerve fiber layer, ganglion cell layer, inner plexiform layer, bipolar cell layer, outer plexiform layer, photoreceptor (rods and cones) layer, and retinal pigment epithelium.
Reminder
Methanol ingestion causes vision loss due to ganglion cell destruction.
The Retina
- The retina contains the cone-rich fovea for color vision and a rod-rich region for non-color vision in low light.
- The macula is responsible for central vision and contains many more cones (color vision) than rods (low light vision).
- The fovea has the highest concentration of cones in the macula.
- The outer retina blood supply is by the choroidal circulation, from short ciliary arteries, which are branches of the ophthalmic artery. The inner retina is supplied by the central retinal artery, also a branch from the ophthalmic artery.
- Central Retinal Artery Occlusion (CRAO): Patients will have painless blindness, with a cherry-red spot and narrowed retinal arteries on the fundoscopic exam.
- Causes of CRAO include increased intraocular pressure, embolism, or decreased venous outflow.
- Spontaneous recovery is called amaurosis fugax.
- The retina is reliant on vitamin A for normal function.
- Vitamin A deficiency is the leading cause of childhood blindness in the world.
- Vitamin A deficiency is the leading cause of childhood blindness in the world.
The Optic disc
- The optic disc is the entry point of the optic nerve into the eye. There are no photoreceptors in the optic disc, and this is the reason for the blind spot in the visual field.
- Increased intracranial pressure can lead to optic disc swelling (papilledema).
- Optic nerve atrophy, as seen after optic neuritis, can cause pallor of the optic disc.
The Pupil and Ocular Autonomic Pathways
- The iris is responsible for controlling the diameter of the pupil, which in turn controls the amount of light that reaches the retina.
- Mydriasis (dilation) and miosis (constriction) of the pupil is dependent on sympathetic and parasympathetic innervation, respectively.
Sympathetic innervation (mydriasis)
- First-order preganglionic neurons from the hypothalamus descend through the lateral brainstem and then synapse in the intermediolateral column of the thoracic spinal cord.
- Second-order preganglionic neurons then project axons to the superior cervical ganglion.
- Axons from the superior cervical ganglia (third-order) neurons travel adjacent to the carotid artery until it diverges within the cavernous sinus. Axons traverse the superior orbital fissure to merge with long ciliary nerves before synapsing on the dilator pupillae muscle.
- Damage along any point of the oculosympathetic pathway (Pancoast tumor, trauma, carotid dissection, etc.) can lead to a Horner’s syndrome (miosis (loss of pupil dilation), ptosis, and anhidrosis).
- Anhidrosis will only occur with 1st order (face and body) or 2nd order (face only) oculosympathetic nerve lesions.
Parasympathetic innervation (miosis)
- Optic nerve fibers synapse on the ipsilateral pretectal nucleus, located in the midbrain.
- Pretectal nucleus neurons then synapse on bilateral Edinger-Westphal nuclei.
- The Edinger-Westphal nuclei are responsible for sending preganglionic parasympathetic fibers to the ciliary ganglia.
- Preganglionic fibers from the Edinger-Westphal nuclei travel via the oculomotor nerve and synapse at the ciliary ganglion.
- Due to the superficial location of these preganglionic fibers along the nerve, mydriasis, due to the lack of parasympathetic output to the pupil, is often the first symptom of cranial nerve III compression (uncal herniation, PCOM aneurysm, etc.)
- Cell bodies within the ciliary ganglion then carry postganglionic parasympathetic fibers via the short ciliary nerve to the sphincter pupillae muscle of the iris, to promote miosis.
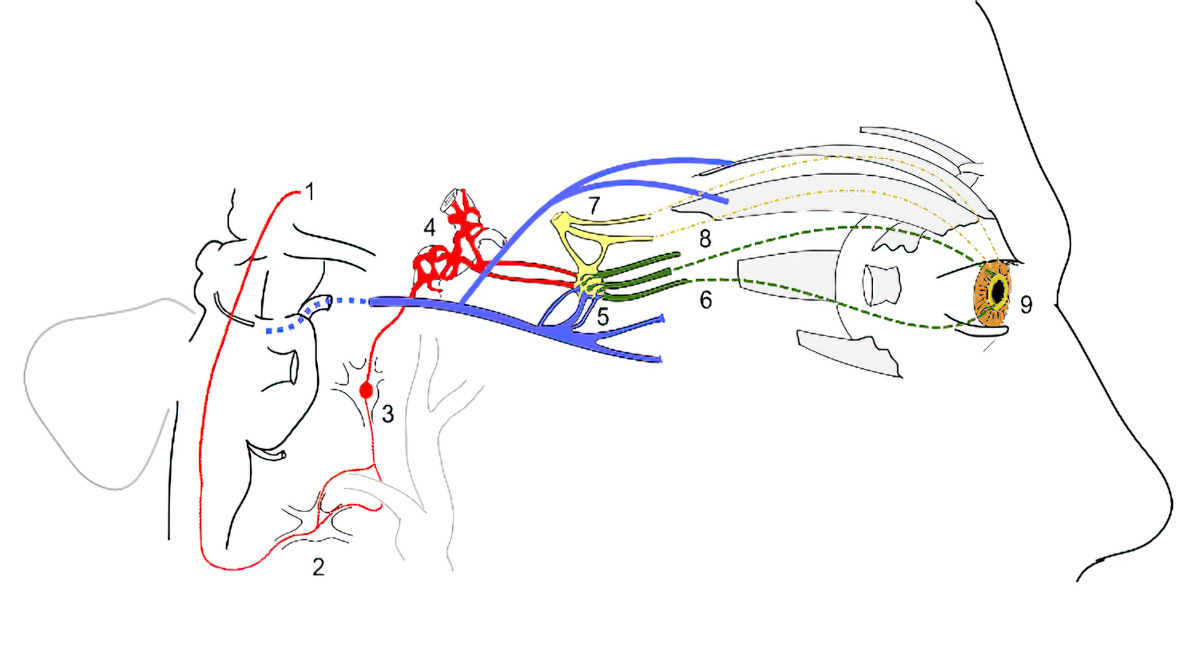
- Preganglionic sympathetic fibers from the thalamus
- Stellate ganglion (no synapse)
- Superior cervical ganglion (sympathetic fibers synapse)
- Carotid plexus with post-ganglionic sympathetic fibers
- Preganglionic parasympathetic fibers (blue) of the oculomotor nerve synapse at the ciliary ganglion
- Postganglionic parasympathetic fibers (dashed green) travel from the ciliary ganglion via the short ciliary nerves to the sphincter pupillae muscle.
- Ophthalmic nerve (yellow) before branching of the long ciliary nerve
- Long ciliary nerve with postganglionic sympathetic fibers (dashed yellow)
- Sphincter pupillae and dilator pupillae muscles of the pupil.