Cranial nerves are a basic neuroanatomy topic that is heavily tested early in clinical training. As one transitions to later phases of their career (internship and residency), the focus moves away from the intricacies of neuroanatomy and more to the associated pathology.
Authors: Brian Hanrahan MD, Steven Gangloff MD
Chapter Multimedia Content
Table of Contents
Table of Contents
The Basics
- Cranial nerves are identified by either their complete name (Olfactory nerve) or by their Roman numeral (Cranial nerve I, CN 1). These terms are used interchangeably throughout this chapter.
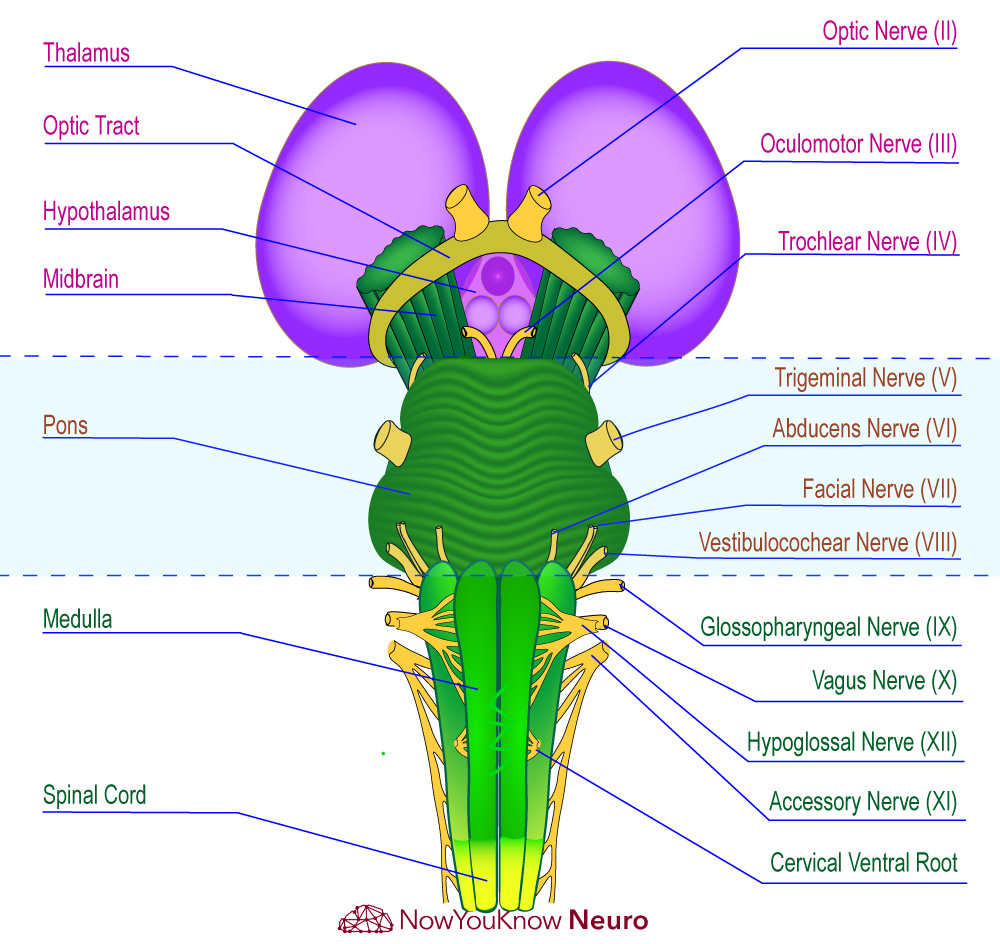
- There are 12 sets of cranial nerves that carry sensory and/or motor fibers.
- Cranial nerves I and II are the only two that do not exit the brain at the level of the brainstem.
- Cranial nerves III and IV exit at the level of the midbrain.
- Cranial nerves V, VI, VII, and VIII exit at the level of the pons.
- Cranial nerves IX, X, XI, and XII exit at the level of the medulla.
- Cranial nerves IV, VI, XI, and XII are pure motor nerves.
- Cranial nerves III, IV, and VI control eye movements and pupillary constriction.
- Cranial nerves I, II, and VIII are pure sensory nerves.
- Cranial nerves V, VII, IX, and X are mixed nerves.
- Cranial nerves III, VII, IX, and X carry parasympathetic fibers.
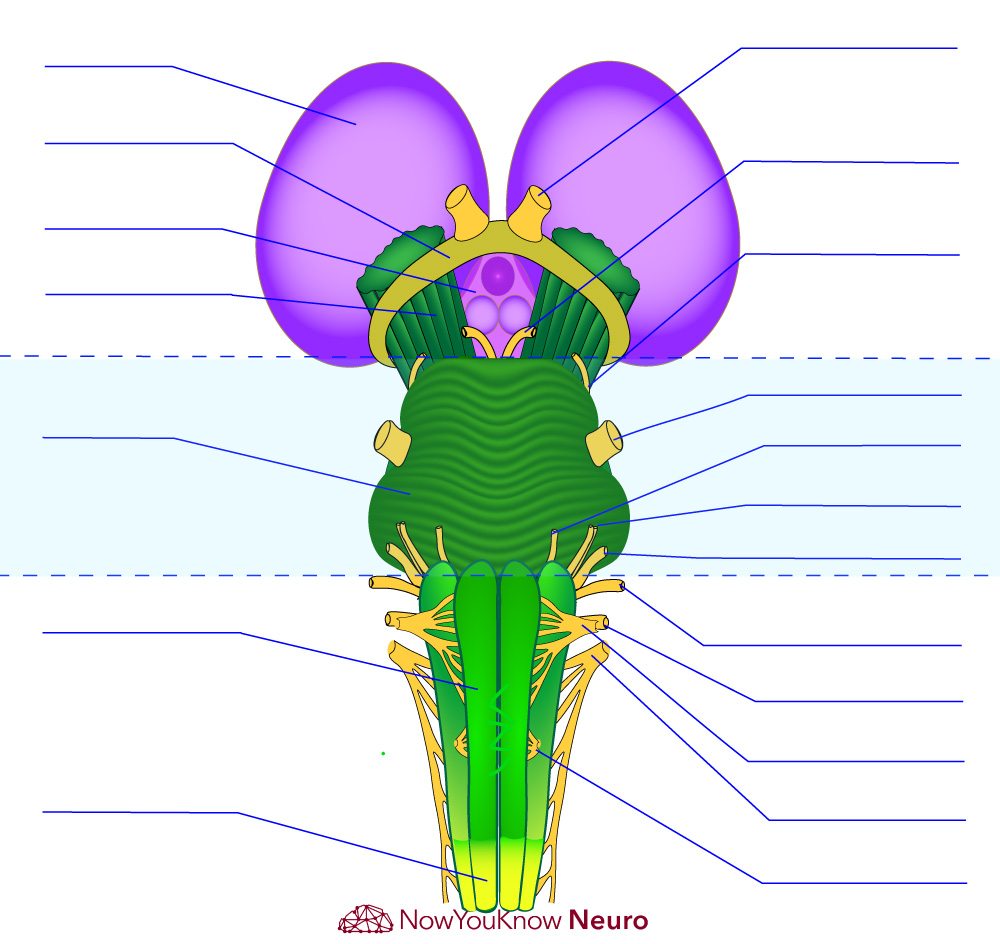
Cranial Nerves & Brainstem Diagram
Move the Slider to Practice!
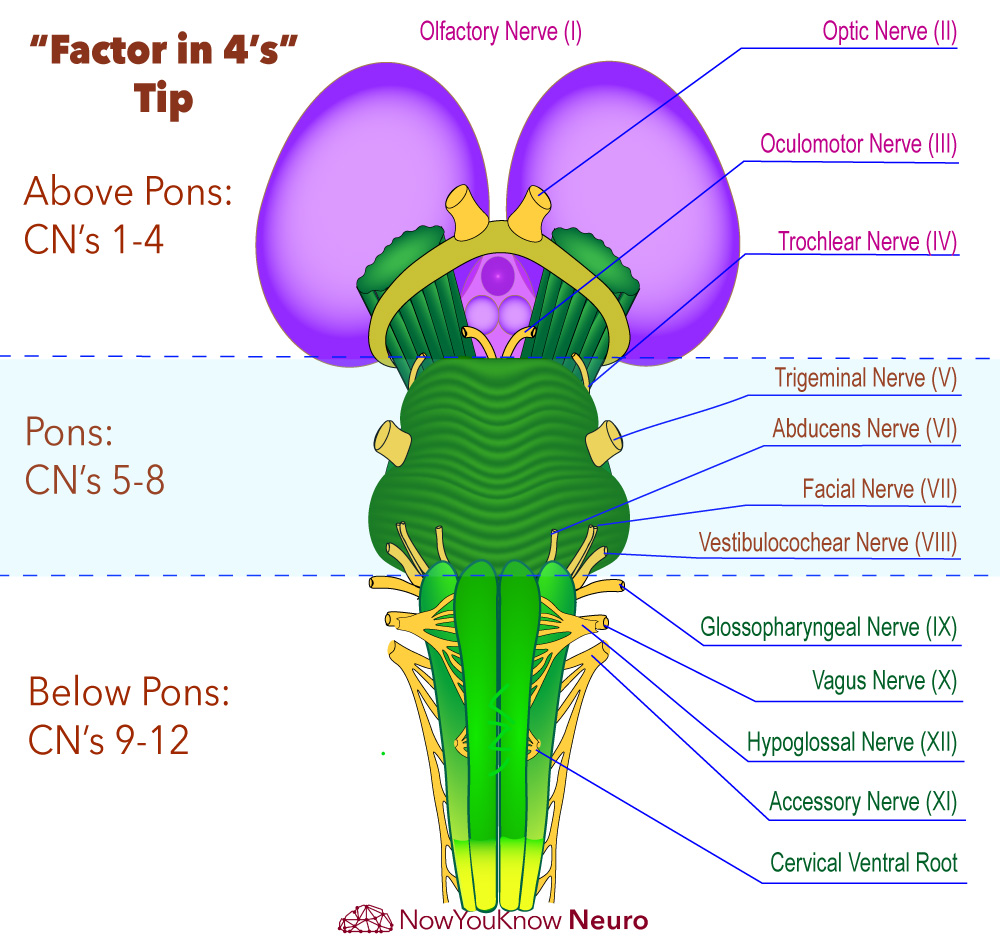
The Factor in 4's Tip
The nuclei of the first four cranial nerves (CN I-IV) exist above the pons (forebrain or midbrain), the next four (CN V-VIII) exist in the pons, and the last four (IX-XII) are located below the pons (medulla or spinal cord).
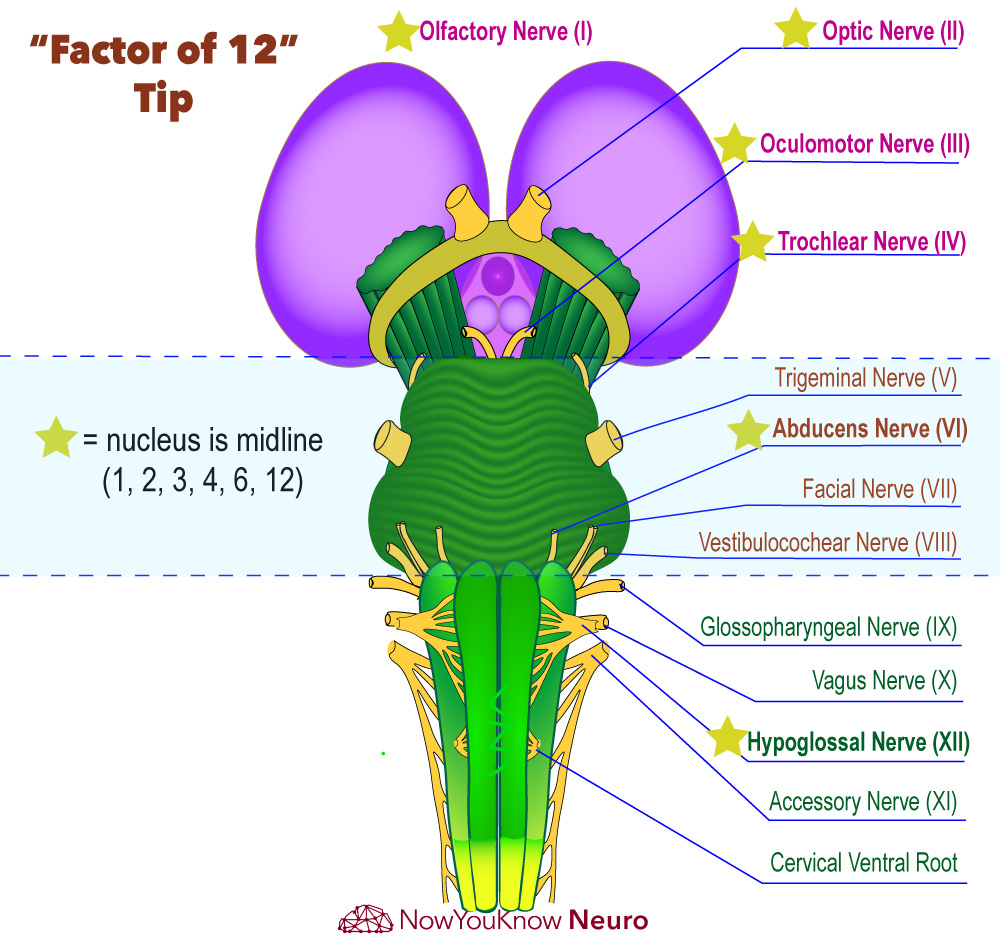
The Factor of 12 Tip
All of the cranial nerves categorized as general somatic efferent (III, IV, VI, and XII) exit the brainstem medially. These are also all of the cranial nerves with nuclei in the brainstem that are factors of the number 12 (i.e. 3, 4, 6, and 12). CN's I and II, are also medial and also a factor of 12, but are not within the brainstem.
Factor in 4's Tip
Factor of 12 Tip
Cranial Nerve I (Olfactory Nerve)
- Sensory: Responsible for the sense of smell.
- Nerve fibers traverse the skull through the cribriform plate where neurons synapse directly with the cortex with no relay through the thalamus.
- Pathology:
- Head trauma can cause damage to the olfactory nerve as it travels through the cribriform plate leading to anosmia.
- Olfactory groove meningiomas can also present with anosmia.
Cranial Nerve II (Optic Nerve)
- Sensory: Responsible for visual sensory input.
Cranial Nerve III (Oculomotor Nerve)
- Motor: Innervates numerous extraocular muscles: superior rectus, inferior rectus, medial rectus, and inferior oblique as well as the levator palpebrae.
- It also provides parasympathetic innervation to the pupillary constrictor and ciliary muscles (the efferent limb of the pupillary reflex).
- Pathology:
- An oculomotor nerve palsy can present with a combination of four possible clinical features; ptosis, ocular deviation, mydriasis, and diplopia.
- Ptosis occurs secondary to the loss of innervation of the levator palpebrae muscle.
- Ocular deviation (down and out) and diplopia occur due to unopposed action of the lateral rectus and superior oblique muscles.
- Mydriasis occurs due to damage to the parasympathetic fibers which supply the pupillary constrictor and ciliary muscles.
- Possible etiologies include trauma, diabetes, hypertension, subarachnoid hemorrhage, and compression from a posterior communicating aneurysm or uncal herniation.
- An oculomotor nerve palsy can present with a combination of four possible clinical features; ptosis, ocular deviation, mydriasis, and diplopia.
NOTE
A posterior communicating artery aneurysm can compress the third cranial nerve leading to ipsilateral pupillary dilatation and ophthalmoparesis.
Cranial Nerve IV (Trochlear Nerve)
- Motor: Innervates the superior oblique muscle, which is responsible for internal rotation and depression of the eye.
- Pathology:
- Exits the brainstem dorsally
- Of the cranial nerves, CN IV has the longest intracranial course.
- Patients will complain of diplopia and difficulty descending stairs.
- On exam, patients will often tilt their head away from (contralateral to) the affected side to compensate for extorsion of the ipsilateral eye.
Cranial Nerve V (Trigeminal Nerve)
- The trigeminal nerve exits the brainstem at the level of the pons and trifurcates into three branches (ophthalmic (V1), maxillary (V2), and mandibular (V3) before exiting the skull.
- The ophthalmic division (V1) traverses the skull through the Superior orbital fissure.
- The maxillary division (V2) traverses the skull through the foramen Rotundum.
- The mandibular division (V3) traverses the skull through the foramen Ovale.
- Mnemonic: “Standing Room Only”
- Sensory: Responsible for all modalities of sensation of the face.
- The ophthalmic division (V1) of the trigeminal nerve innervates the scalp, forehead, upper eyelid, conjunctiva and cornea of the eye, and the meninges.
- The maxillary division (V2) supplies sensory innervation to the lower eyelid and cheek, upper lip, upper teeth, gums, the nasal mucosa, the palate, and the roof of the pharynx.
- The mandibular division (V3) provides sensation to the cheek, the external auditory meatus, the tympanic membrane, the lower teeth and gums, the anterior 2/3 of the tongue, the lower lip, and the chin.
- Motor: Innervates the muscles of mastication (masseter, temporalis, medial, and lateral pterygoids), tensor veli palati, anterior belly of the digastric, mylohyoid, and tensor tympani.
- The motor fibers of the trigeminal nerve exit the skull via the foramen ovale along with the other mandibular division (V3) fibers.
- Pathology:
- Associated symptoms with a trigeminal lesion include impaired facial sensation and impaired hearing of the ipsilateral ear secondary to damage to the tensor tympani muscle.
- These symptoms can be seen in Wallenberg’s syndrome which is due to damage to the lateral medulla from a posterior inferior cerebellar artery (PICA) ischemic stroke.
- Trigeminal neuralgia (Tic douloureux):
- Compression of the trigeminal nerve can lead to trigeminal neuralgia which presents with intermittent, severe sharp/stabbing-like paroxysms of the face. Episodes usually occur for only a few seconds at a time.
- The sensory examination of the face is typically normal.
- Common triggers for pain include brushing teeth, washing the face, and strong winds hitting the face.
- Carbamazepine is the first-line therapy.
- Associated symptoms with a trigeminal lesion include impaired facial sensation and impaired hearing of the ipsilateral ear secondary to damage to the tensor tympani muscle.
Remember
The dura of the anterior fossa is predominantly innervated by the ophthalmic branch of the trigeminal nerve (CN V1), and the posterior fossa is predominantly innervated by cervical roots C2 and C3, as well as CN X.
Log in to View the Remaining 60-90% of Page Content!
New here? Get started!
(Or, click here to learn about our institution/group pricing)1 Month Plan
Full Access Subscription
$142.49
$
94
99
1 Month -
Access to all chapters
-
Access to all images and cases
-
Access to all flashcards
-
Access to Full Question Bank
3 Month Plan
Full Access Subscription
$224.98
$
144
97
3 Months -
Access to all chapters
-
Access to all images and cases
-
Access to all flashcards
-
Access to Full Question Bank
1 Year Plan
Full Access Subscription
$538.47
$
338
98
1 Year -
Access to all chapters
-
Access to all images and cases
-
Access to all flashcards
-
Access to Full Question Bank
Popular